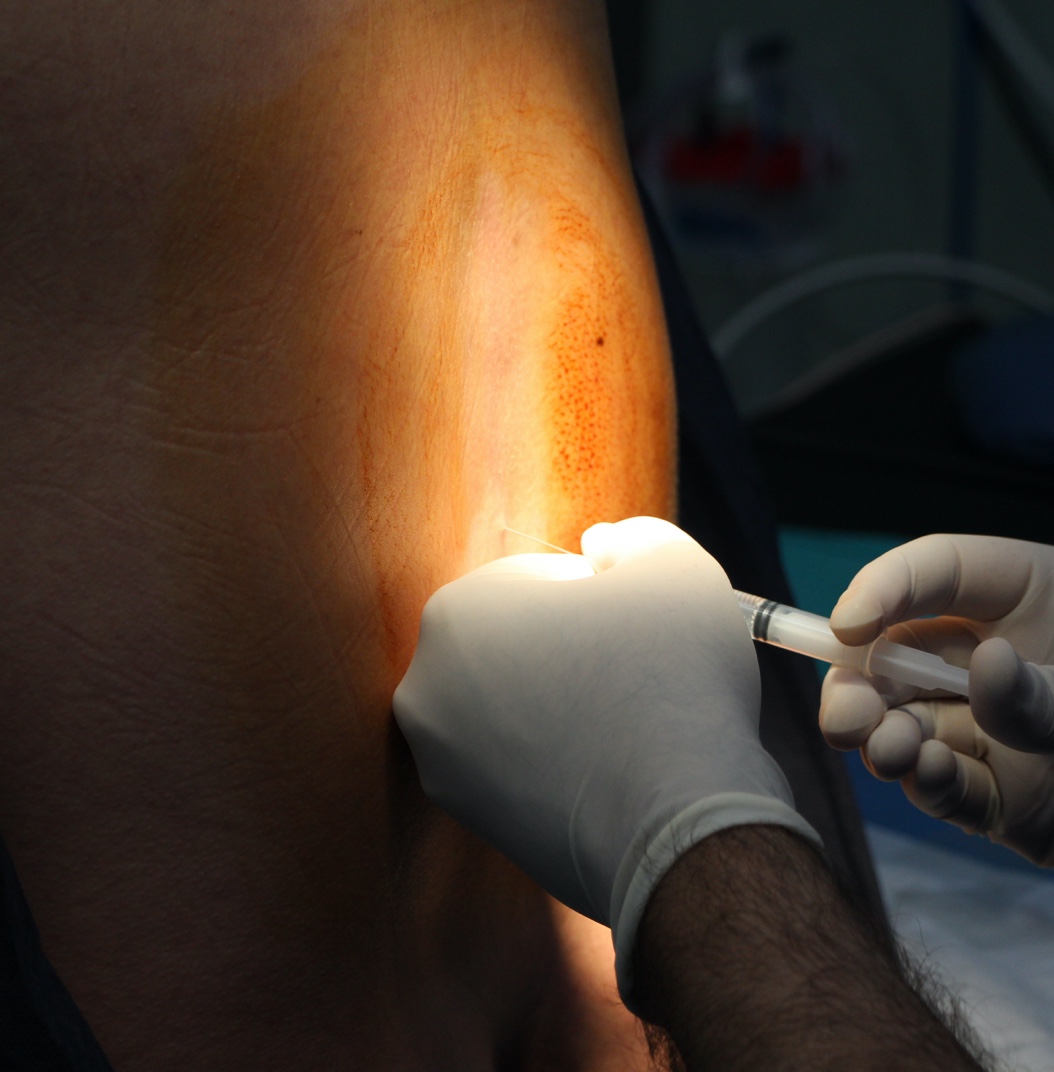
Epidural procedures are a popular way to help patients feel less pain during childbirth or other surgeries, but are they truly safe?
Let’s examine the effects of this modern medicine marvel known as the epidural.
What is an Epidural?
An epidural inhibits pain signals in certain parts of the body by temporarily numbing the spinal cord. This injection goes into what’s known as your “epidural space,” located right outside of the spinal cord membrane.
Doctors use epidurals to aid in pain relief during and after a surgery, especially when managing chronic pain. It can provide a longer-lasting pain relief, and because it requires a lower than normal dose of medicine, patients don’t feel “drugged out” afterwards. They can remain more mobile after surgery.
What is an Epidural Most Commonly Called?
Some of the most common phrases associated with epidurals include: epidural steroid injection (ESI), epidural block, epidural anesthesia, and regional anesthesia.
Epidural Steroid Injection (ESI)
This process injects both a corticosteroid and an anesthetic numbing agent into the epidural space within the spine.
These injections work to lessen inflammation and are great when sent right into the most painful area. Pain relief can last anywhere from a few days to a few years.
ESI is most commonly used for patients with spinal stenosis, degenerative discs or sciatica.
Epidural Block
Epidural blocks are the treatments used in pregnancy to reduce pain during childbirth. It can also reduce pain in the lower extremities during surgery.
It’s common for patients to shiver after receiving an epidural but this does not warrant concern. Many women shiver during labor with or without this procedure.
Two of the main types of epidural blocks are the “walking” epidural block and the combined spinal epidural block. The former allows patients to move their legs while still alleviating some pain, while the latter provides pain relief much faster and is usually needed when women are right in the middle of labor.
Epidural Anesthesia
Epidural anesthesia is the most popular method of pain relief during the labor process. This is the one you are likely most familiar with.
Numbing occurs within just a few minutes following the initial placement of the epidural, and women typically feel the entire numbing effect after 20 minutes.
Regional Anesthesia
Instead of making the entire body numb, regional anesthesia only makes certain parts of the body numb.
This could be used in both male and female reproductive surgery environments as well as for orthopedic surgeries.
Epidural anesthesia is one subset of regional anesthesia, focusing on the cluster of nerves in the lower back.
What Happens During an Epidural Injection?
Epidurals usually begin with a conscious sedation process, allowing the patient to feel relaxed while technically awake during their procedure.
Next the physician uses their advanced medical technology to guide a small needle into the epidural space.
Following the surgery, it’s best for the patient to organize a ride home since it may take several hours for the effects of treatment to fully wear off.
What is an Epidural Nerve Block?
An epidural nerve block works quickly to numb the spinal nerves and keep pain signals away from the brain. The patient is still able to feel the sensation of touch.
The nerve block is done via a catheter that goes near the spine and delivers the medicine without a stoppage. This ensures that the patient will never experience pain during the surgery.
Other epidural injections may be done using different medications like steroids.
What is an Epidural with Patient-Controlled Analgesia (PCA)?
There is an option for allowing patients to control the amount of pain relief they will receive via their epidural catheter. Called patient-controlled analgesia, this PCA pump ensures that a patient only receives medication when they feel pain by allowing the patient to press a button. It’s initially configured by the healthcare provider based on the patient’s needs. The pump won’t administer the medication when it’s not time to receive another dose.
What are the Most Common Conditions Treated by an Epidural Injection?
There are several use cases for an epidural injection, including conditions like a pinched nerve, herniated disc, or spinal stenosis. For many people, pain relief can last multiple months.
Who Performs an Epidural?
Certified specialists, usually an RN anesthetist or anesthesiologist performs the procedure. An anesthesiologist is someone who cares for patients throughout the surgery process, before, during, and after. They are specially trained to inject the anesthesia and attend to the patient’s needs at all times.
Thanks to many innovations in modern medical technology, the ability of anesthesiologists to properly attend to all the needs and issues experienced by their patients has never been easier.
Epidurals have never been safer just as modern medical environments have never been safer.
What are the Risks of Epidurals?
Although epidurals are incredibly common and safe, there are some unusual risks that all patients should be aware of.
Risk of Nerve Damage
The biggest potential risk is faced in the beginning, with the way an epidural is administered. Individuals can face permanent nerve damage if the epidural is not placed correctly by the doctor.
The needle used to deliver the epidural may hit a nerve which can lead to paralysis in the lower body. Bleeding in the spinal cord area is another potential hazard that can cause nerve damage.
Thankfully, it’s extraordinarily rare for nerve damage to happen during an epidural. Roughly one in several hundred thousand people experience this.
Risk of Infection
Introducing a foreign object into the skin, like a needle, can cause bacteria to enter. Although rare, this can result in an infection which has the potential to spread to other parts of the body if not treated immediately.
Risk of Breathing Difficulties
Once the anesthesia takes effect, there’s an unlikely chance it could negatively affect the chest muscles and inhibit breathing.
Some people experience a mucus build-up in their lungs because of the anesthesia. It can cause them to feel pain whenever they attempt to send air out of their mouth or even breathe normally.
In ultra-rare cases, the patient could have a collapsed lung combined with a rapid heart rate.
Risk of Hyperthermia
Malignant hyperthermia is another very unusual risk that can occur during surgery. This involves a sudden onset fever accompanied by muscle contractions. It is most closely associated with people who have previously suffered a heat stroke or who have had malignant hyperthermia before.
How Can Assisted Epidural Placements Help?
An assisted epidural placement makes the injection process safer and all but eliminates potential risk factors. These tools help anesthesiologists lessen the risk of dural punctures and make the epidural administration process a lot smoother.
One example of this is the CompuFlo Epidural Instrument which is able to detect pressure changes and determine the correct epidural space within a matter of minutes helping physicians do their job with greater precision.
These devices are responsible for making modern medical technology even safer and more reliable for all.
What are The Side Effects of an Epidural?
Aside from the above mentioned risk factors, here are some fairly common effects that are non-life threatening. It’s important to note that none of these side effects of the epidural impact the baby or affect the pregnancy.
Decrease in Blood Pressure
As the body is relaxing, there may be a drop in blood pressure following epidural administration. If this happens during childbirth, there is a risk that the baby’s heart rate may be slowed which would need to be remedied by receiving extra fluids and having the mother lie on her side.
Headache
Headaches are on the rare end of the epidural side effects spectrum, and may result from the epidural injection puncturing the protective layer of the spinal cord. This happens in a very small percentage of overall cases.
Numbness
Epidural long term side effects in the legs are rare, but it’s possible that some women may feel tingling or numbness in their legs following injection. Luckily this should subside shortly after the child is born.
Back Pain
Soreness in the back area happens because this is the injection site. This type of pain shouldn’t last more than a few days.
Difficulty Urinating
If the person is struggling to urinate for a prolonged period of time following the epidural, they may require a urinary catheter.
What Risk Factors Make Epidurals More Dangerous?
There are certain risk factors that can increase the chances of a patient experiencing a negative side effect from an epidural, among them are:
- Allergies
- Diabetes
- Previous kidney problems
- Obesity
- Stroke
- Asthma
- Chronic Obstructive Pulmonary Disease (COPD)
- Seizure
- Excessive drinking
How Can Epidurals Side Effect Profiles be Lessened?
Similarly, to the risks previously mentioned, these side effects can be all but eradicated thanks to modern technology like the CompuFlo Epidural System or CathCheck Verification System (helps physicians verify the placement of a catheter).
Of course, there are outliers and anomalies that are out of anyone’s control, but this new technology continues to make epidurals an even safer process for all.
Potential Epidural Side Effects Long Term
To be clear, long-term side effects from an epidural are extremely rare, regardless of the patient’s pre-existing conditions.
If long-term side effects of epidural steroid injections are to happen, they usually involve one of the following:
- Nerve root damage in the spinal cord, caused by injection.
- Hematoma leading to paralysis, caused by an accumulation of blood between the spine and the dura mater.
- Lower back pain, or other back problems that cycle on and off indefinitely.
- Sciatica caused by a buildup of gas within the spine
These long-term effects are so uncommon that most anesthesiologists won’t need to consider them when deciding whether to administer an epidural.
The most common side effects go away within hours following the procedure, and there is little to no chance of risk posed to the newborn child. Epidural side effects after birth are extremely uncommon.
Once again, it’s the work of modern medical technology to ensure a more targeted drug delivery system that keeps these long-term side effects very rare.